An objective summary of the paper
I’m going to be discussing this paper from Du et al., 2024, but first I want to give a little primer on fluid transport systems in the body. Otherwise, I don’t think this post will make much sense…
Fluid transport systems in the body
Cardiovascular and lymphatic systems
Fluids in the body typically get transported in specialised transport systems, the most obvious being the cardiovascular system, which typically transports blood, water, and essential metabolites and nutrients through blood vessels to tissues. Another system is the lymphatic system. The lymphatic system, made of lymphatic vessels and lymph nodes, is important for regulating immune function, fluid balance, and removal of waste including cellular debris, lipids, proteins, and other waste products from tissues.
While the cardiovascular and lymphatic systems have some structural similarities, they also have important differences. Both systems have vessels that transport fluids, but lymphatic vessels are generally thinner and have a more irregular structure compared to blood vessels (Figure 1). Lymphatic vessels, like some blood vessels, contain smooth muscle cells and valves to maintain unidirectional movement of lymph - which is a fluid composed mostly of water, proteins, cellular waste, and immune cells.
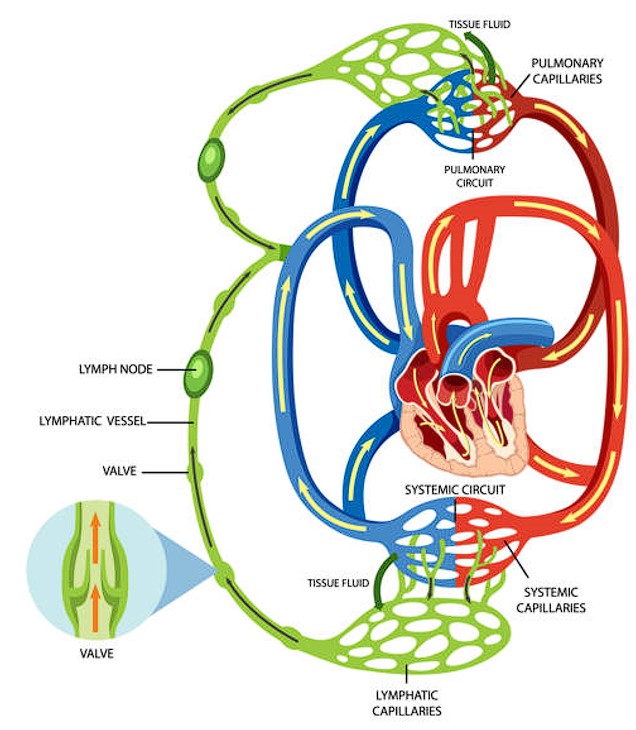
These two systems support each other - where the cardiovascular system can be the waterworks providing you with clean water, the lymphatic system can act as your drainage system. This is a simplified analogy, as the cardiovascular system also removes waste, and the lymphatic system can provide nutrients, but for the sake of this post, we’ll keep it simple.
Glymphatic system
The brain has its own specialised transport systems. The brain sits in cerebral spinal fluid (CSF). CSF is similar to blood, it’s mostly composed of water, glucose, proteins, metabolities and nutrients that are needed for the brain to function. However, unlike blood, it does not contain any red blood cells, and so it is a clear and colourless fluid.
The glymphatic system, termed after glia (brain cells) + lymphatics, hypothesises that CSF is moved around the brain along perivascular spaces and through periarterial pulsations, where it then mixes with the brain interstitium (tissue) via bulk/convective flow (Figure 2). During which nutrients can be spread in the brain, and importantly waste products can be removed. The removal of this waste is then via multiple mechanisms which are still been explored. There is still ongoing debate about the existence of the glymphatic system, and I will likely discuss it in a future post, but for now let’s assume it exists, and we can ask the question: how does CSF get cleared from the brain?
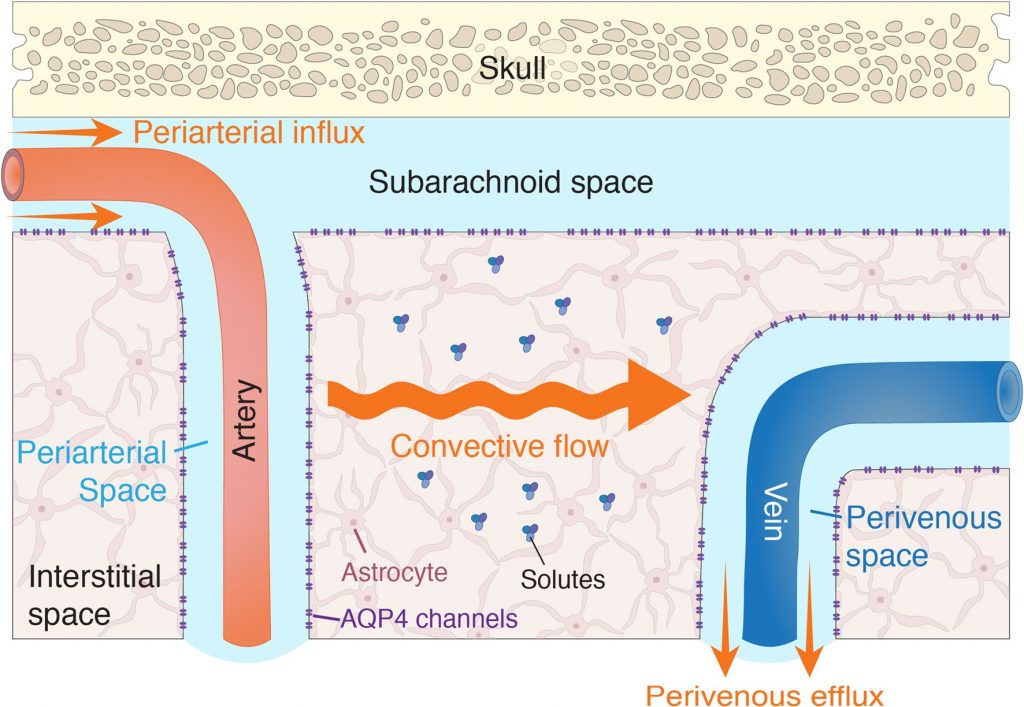
It has been thought for a while that the brain lacks a functioning lymphatic system, which is bizarre when you think about it, until the lab of Jonathan Kipnis showed that indeed lymphatic vessels do exist in the brain (Louveau et al., 2015). Which ties it nicely with the glymphatic system. CSF could also be drained through brain lymphatic vessels.
Impairments in glymphatic and brain lymphatic vessels have been observed in Alzheimer’s disease, Parkinson’s disease, stroke, and traumatic brain injury, and although most of the evidence is in animal models, we can extrapolate to human conditions and attempt to find treatments by manipulating these systems. Therefore, Du et al., (2024) demonstrated that therapeutically targeting cervical lymphatic vessels can rescue CSF drainage in the ageing brain. Which is important, because we do not want waste accumulating in our brains. This can lead to very nasty outcomes.
Study methods
Du et al., (2024) designed a 2-photon imaging technique, 2P-OPTIC, that allows them to visualise particles in the CSF and the lymph of peripheral lymphatic vessels in live mice (Figure 3, left). This then allowed them to see the movement of CSF particles into the cervical lymph, and investigate the function of lymphatic vessels by measuring the volume and rate of clearance of CSF particles. Importantly, they could do this in real-time (Figure 3, right).
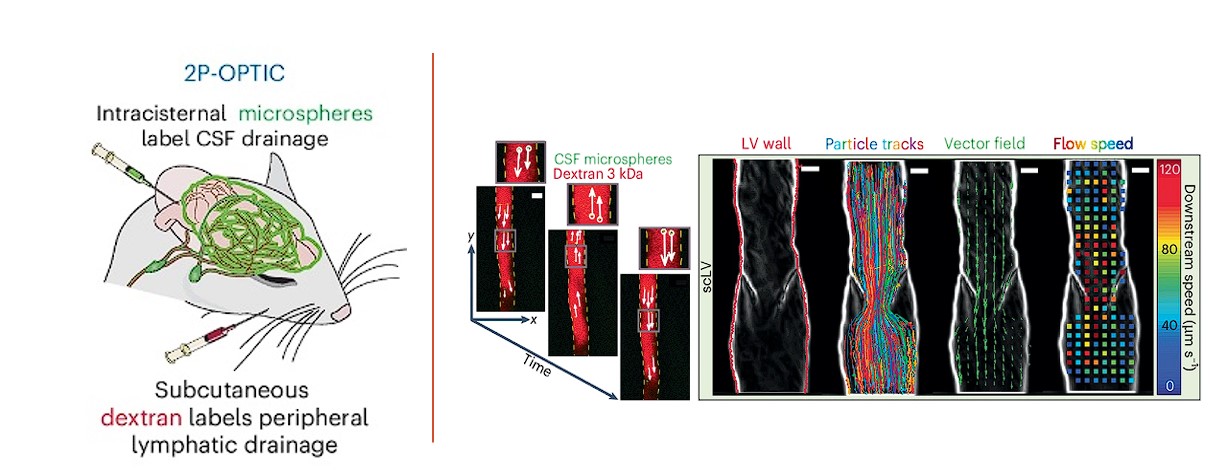
Study results
Using this system they found that lymphatic vessels in aged animals had reduced frequency and amplitude of lymphatic contractions (Figure 4). This was due to faulty lymphatic valves that failed to open and close properly, and loss of smooth muscle cells.
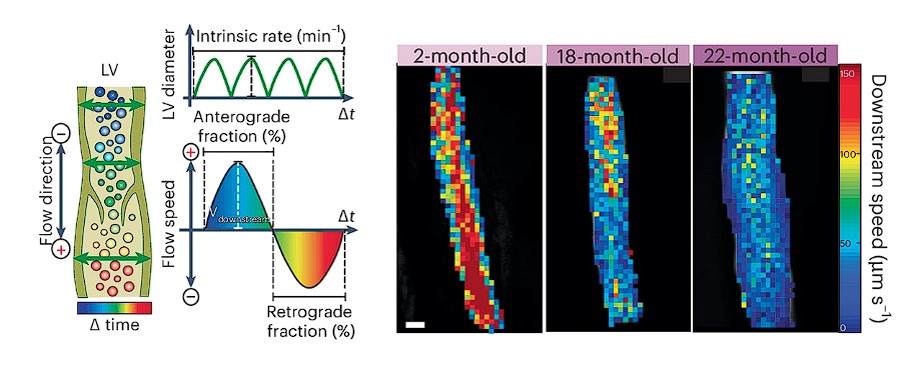
Interestingly, they found that topical administration of prostaglandin F2ɑ’ (PGF2α) directly on cervial lymphatic vessels rescued function of these lymphatic vessels in ageing animals, resulting in increased CSF drainage from the brain (Figure 5). PGF2α is known as dinoprost and is used to induce labour in women and also as an abortifacient. Equally, PGF2α treatment in young animals increased CSF drainage, although not to the same extent as in older animals. This result shows that cervical lymphatics are important drivers of CSF clearance.
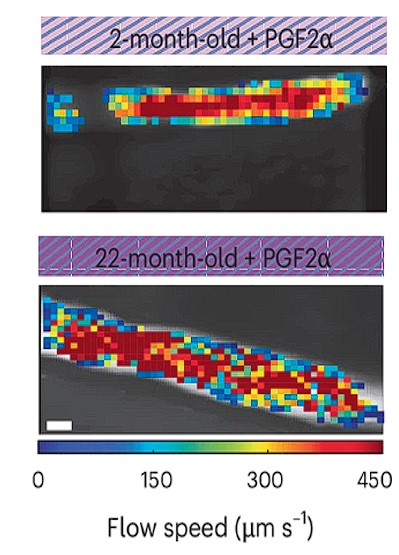
Conclusions
Du et al., (2024) elegantly demonstrated that CSF drainage is impaired with ageing and this can be rescued by topical administration of PGF2α.
My thoughts
To the glymphatic field, I believe this is an incredibly important paper. If we consider the glymphatic system to be in three stages: 1) glymphatic influx, 2) fluid exchange, and 3) glymphatic outflow, this paper neatly demonstrates these three processes using a quantitative, real-time technique in 2P-OPTIC.
As the authors discussed, the strengths of this method is that its in vivo, its high resolution, and its detection of multiple dyes, however it requires the need to inject exogenous dyes. My understanding is that these procedures are non-recovery, i.e. the animals do not wake up after the procedure. Although, that said, the results reported are very important in further understanding the systems involved in brain clearance.
Previous studies have shown ablation of cervical lymphatic vessels is sufficient to worsen Alzheimer’s disease pathology by disruption of the glymphatic system, and treatment of aged lymphatic vessels with PGF2α could improve glymphatic function - it would be interesting to see the use of PGF2α treatment in an alternative disease model.
Lastly, PGF2α induces contraction of smooth muscle cells, these also form blood vessels, and as already shown, by the same authors, activation of smooth muscle cells can enhance glymphatic function Holstein-Rønsbo et al. 2023. Could off-target/unintended effects of PGF2α resulted in improved brain clearance?
How does this work benefit society?
As mentioned, impaired glymphatic function has been described in ageing, and ageing related disorders. As populations continue to age, and life expectancy continues to rise - ageing will/is already causing large economic burden, particularly to developed nations. And therefore, studies like the one presented here are incredibly important in furthering our understanding of potential treatments for ageing-related disorders.
I appreciate that Du et al., (2024) chose to use an already marketable treatment in PGF2α. Repurposing of drugs is important because it reduces the development time from bench to bedside, it reduces risk as it has already been tested for safety, and ultimately increases the success rate of the treatment.
Papers like this are a joy to read, and I would highly recommend it to anyone interested in the field of ageing research.
 Science #1: Organ aging signatures in the plasma proteome track health and disease
Science #1: Organ aging signatures in the plasma proteome track health and disease
